Prediction of Early Neurological Deterioration in Individuals With Minor Stroke and Large Vessel Occlusion Intended for Intravenous Thrombolysis Alone. Seners P, Ben Hassen W, Lapergue B, Arquizan C, Heldner MR, Henon H, Perrin C, Strambo D, Cottier JP, Sablot D, Girard Buttaz I, Tamazyan R, Preterre C, Agius P, Laksiri N, Mechtouff L, Béjot Y, Duong DL, Mounier-Vehier F, Mione G, Rosso C, Lucas L, Papassin J, Aignatoaie A, Triquenot A, Carrera E, Niclot P, Obadia A, Lyoubi A, Garnier P, Crainic N, Wolff V, Tracol C, Philippeau F, Lamy C, Soize S, Baron JC, Turc G. JAMA Neurol. 2021 Jan 11;. doi: 10.1001/jamaneurol.2020.4557. [Epub ahead of print] PubMed PMID: 33427887. Download from HAL-INSERM
Cet article est issu de la cohorte multicentrique MINOR-STROKE que Pierre et moi coordonnons. Il étudie la détérioration neurologique précoce post-thrombolyse intraveineuse chez les patients présentant un déficit neurologique mineur et une occlusion proximale, et montre les résultats suivants :
1) 13% des patients présentent une détérioration neurologique précoce, qui est d’origine « ischémique » dans 90% des cas (très rares aggravations hémorragiques dans cette population)
2) Cette détérioration neurologique « ischémique » est très fortement associée à un mauvais pronostic à 3mois, y compris en cas de thrombectomie « de sauvetage »
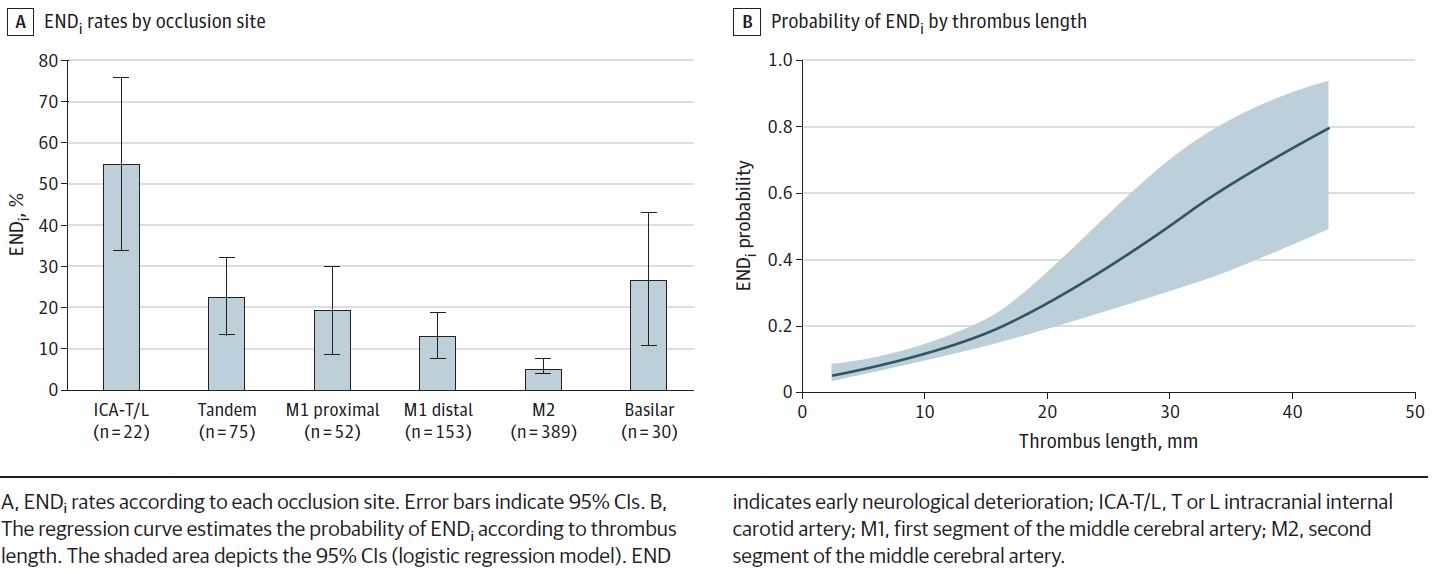
3) Les 2 seuls facteurs prédictifs indépendants de détérioration neurologique identifiés sont le site de l’occlusion artérielle et la longueur du thrombus (à savoir, les marqueurs de non-recanalisation post-thrombolyse)
4) Un score prédictif d’aggravation clinique, basé sur ces 2 variables, permet une prédiction satisfaisante de cette aggravation, sur 2 larges cohortes indépendantes.
Abstract
Importance: The best reperfusion strategy in patients with acute minor stroke and large vessel occlusion (LVO) is unknown. Accurately predicting early neurological deterioration of presumed ischemic origin (ENDi) following intravenous thrombolysis (IVT) in this population may help to select candidates for immediate transfer for additional thrombectomy.
Objective: To develop and validate an easily applicable predictive score of ENDi following IVT in patients with minor stroke and LVO.
Design, setting, and participants: This multicentric retrospective cohort included 729 consecutive patients with minor stroke (National Institutes of Health Stroke Scale [NIHSS] score of 5 or less) and LVO (basilar artery, internal carotid artery, first [M1] or second [M2] segment of middle cerebral artery) intended for IVT alone in 45 French stroke centers, ie, including those who eventually received rescue thrombectomy because of ENDi. For external validation, another cohort of 347 patients with similar inclusion criteria was collected from 9 additional centers. Data were collected from January 2018 to September 2019.
Main outcomes and measures: ENDi, defined as 4 or more points' deterioration on NIHSS score within the first 24 hours without parenchymal hemorrhage on follow-up imaging or another identified cause.
Results: Of the 729 patients in the derivation cohort, 335 (46.0%) were male, and the mean (SD) age was 70 (15) years; of the 347 patients in the validation cohort, 190 (54.8%) were male, and the mean (SD) age was 69 (15) years. In the derivation cohort, the median (interquartile range) NIHSS score was 3 (1-4), and the occlusion site was the internal carotid artery in 97 patients (13.3%), M1 in 207 (28.4%), M2 in 395 (54.2%), and basilar artery in 30 (4.1%). ENDi occurred in 88 patients (12.1%; 95% CI, 9.7-14.4) and was strongly associated with poorer 3-month outcomes, even in patients who underwent rescue thrombectomy. In multivariable analysis, a more proximal occlusion site and a longer thrombus were independently associated with ENDi. A 4-point score derived from these variables-1 point for thrombus length and 3 points for occlusion site-showed good discriminative power for ENDi (C statistic = 0.76; 95% CI, 0.70-0.82) and was successfully validated in the validation cohort (ENDi rate, 11.0% [38 of 347]; C statistic = 0.78; 95% CI, 0.70-0.86). In both cohorts, ENDi probability was approximately 3%, 7%, 20%, and 35% for scores of 0, 1, 2 and 3 to 4, respectively.
Conclusions and relevance: The substantial ENDi rates observed in these cohorts highlights the current debate regarding whether to directly transfer patients with IVT-treated minor stroke and LVO for additional thrombectomy. Based on the strong associations observed, an easily applicable score for ENDi risk prediction that may assist decision-making was derived and externally validated.
This part of the website could either be in French or English, depending on the sources of the actualities.